

From WPC 2023


From WPC 2023
A gallop around the posters
Jonathan Bromley
Here’s a little maths puzzle for you. WPC had 750 poster papers, and I had two 60-minute lunch breaks to see them all. How long did I have to look at each poster?
To save you the headache I did the sums for you: it’s 9½ seconds.
Less than ten seconds to consider a poster describing work that probably had occupied a team of people for months. Oof.
I scurried around the poster displays, elbowing my way through the crowds and rapidly ignoring…
And then I got busy with the phone camera, snapping as many as I could so that I might follow up later. I thought I had recorded many dozens. Looking at my photos now, in fact I have only about twenty. The big problem, of course, was that as soon as something really caught my eye I would start chatting with one of the poster’s presenters, and that would burn up another three or four minutes. Whoops, each of those 4-minute chats represented 24 more posters I didn’t have time to see.
Like almost everything at WPC, the posters filled me with joy at the volume, intensity and vibrancy of work that’s going on to improve lives of those living with Parkinson’s. Posters covered every imaginable aspect of the condition: basic science, drug development, treatment options, best practice in care, the role of care partners, patient involvement, opportunities offered by new technology, and mutual support in local and worldwide communities. A handful of recurring themes caught my untrained eye. I’m sure I missed far more than I saw, but here is my very personal summary.
Dyskinesia is an uncontrolled jerky swaying or rolling movement that some people with Parkinson’s experience. It seems to arise after many years of levodopa treatment. At present the only approved medication is a drug called amantadine, which has worked well for many (including Sally) but has limited value or undesirable side-effects for others.
A team from various universities in Sweden, along with startup pharma company Neurolixis, presented encouraging results from a new drug NLX-112, also known as befiradol. The study, funded by Parkinson’s UK and Michael J Fox Foundation, showed not only good control of dyskinesia but also improvements in other motor symptoms. This might allow patients to cut back on levodopa medication, as well as easing their dyskinesia.
At Lille CHU (University Hospital) in France, a group working with startup company InBrain Pharma has developed a form of levodopa that can be fed straight into the brain using a small pump. A small trial with 10 patients has shown promising results, greatly reducing the need for conventional levodopa medication and thus helping with dyskinesia. It’s a rather invasive and burdensome treatment, though, and doesn’t look like something that will be widespread in its present form.
Groups all over the world are working on using technology to track Parkinson’s progression, support clinical decision-making, predict adverse events such as falls, and improve research studies. As I’ve said elsewhere, the landscape is fragmented and almost chaotic at present, with academics and commercial operations all trying various ways to take advantage of the eye-watering possibilities that come with almost everyone having a sensor-packed, internet-connected smartphone in their pocket.
Several posters discussed how to get good information from simple non-intrusive measurements. Can we use the quality of a patient’s voice to track their Parkinson’s progression? Can falls and freezing be predicted from routine measurement of your steps using the phone in your pocket? The answer seems to be: yes, probably, but we will need a lot more understanding, and a lot of artificial intelligence (AI), to get really useful information.
This is an incredibly exciting field, with advances in AI being picked up and applied at breathless pace by companies and researchers. How it’s going to work in practice, for real patients and real clinicians, is not so clear just yet. With our close links to local startups NeuHealth and GaitQ, Oxford Branch is in a great position to keep track of these developments.
Many posters showed the richness of the Parkinson’s community in all its forms. Patient involvement was a strong theme, along with brilliant international efforts to level-up Parkinson’s care across the world.
We met Kabugo Hannington Tamale, a leader in Parkinson’s Africa. He received a WPC Outstanding Community Service award for his amazing work in Uganda to inform, educate, and reduce the stigma of Parkinson’s found in many rural communities. He is also working with partners worldwide to help improve access to Parkinson’s medication and support in Africa. Richard Walker and Natasha Fothergill-Misbah of Newcastle University presented breathtakingly ambitious plans to support this work in numerous countries across the continent.
A number of community-oriented posters looked at issues that are directly relevant to our Branch: managing succession in group leadership, reaching under-represented communities, and supporting care partners. Are we doing enough to stay connected with like-minded individuals and organizations so that we can be more effective together?
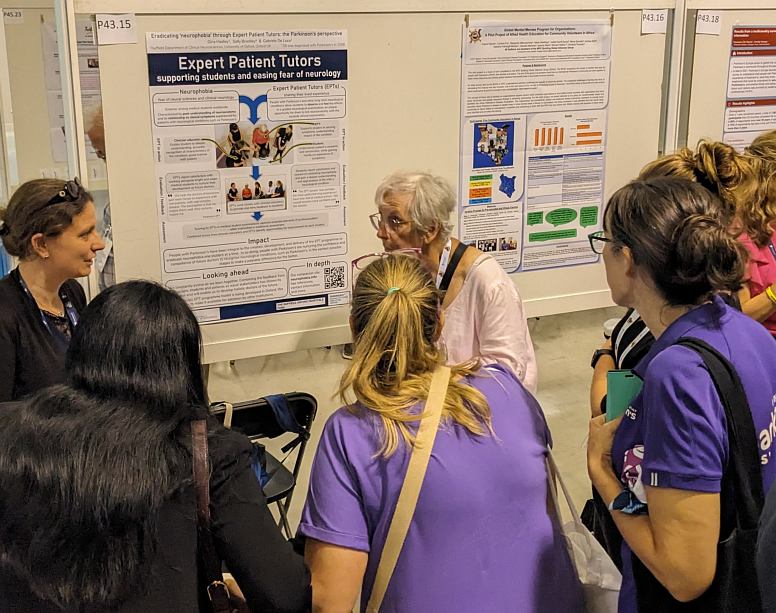
Finally, and closer to home, this poster from Sally, Gabe de Luca and Gina Hadley describing Expert Patient Tutors at the John Radcliffe Hospital drew a lot of interest. It featured on one of the Poster Tours that led visitors around the steering committee’s choice of best posters.
Parkinson's UK is the operating name of the Parkinson's Disease Society of the United Kingdom.
A registered charity in England and Wales (258197) and in Scotland (SC037554). 50 Broadway, London SW1H 0BL.